
Screening for Colorectal Cancer
Regular screening will discover polyps before they start developing colorectal cancer
-
Identifying Risk Factors
Screening
Treatment
Screening Options
There are various screening options available – the main ones are described below. To decide which screening option is right for you, please talk to your doctor.
Stool Tests
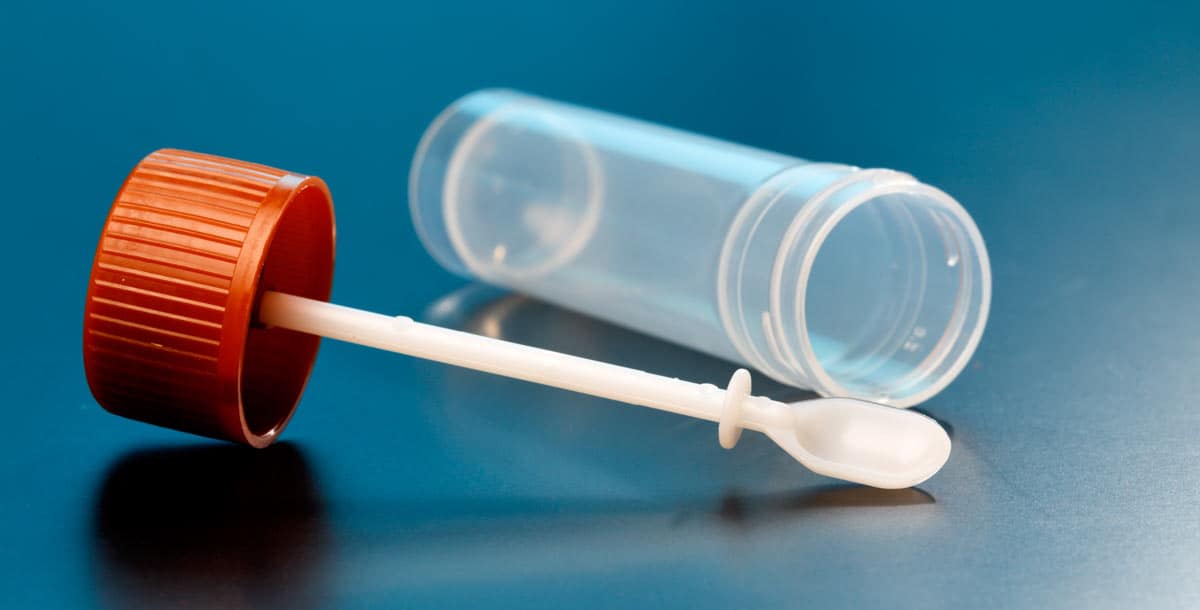
A stool test is any easy test that checks your stool for blood. Some people find this embarrassing but it could save your life – it is that simple. Polyps or cancer in the colon or rectum have blood vessels that may release a small amount of blood that is picked up by the stool as it passes through the colon. Stool tests check for traces of this hidden (occult) blood which cannot be seen by eye.
FOBT
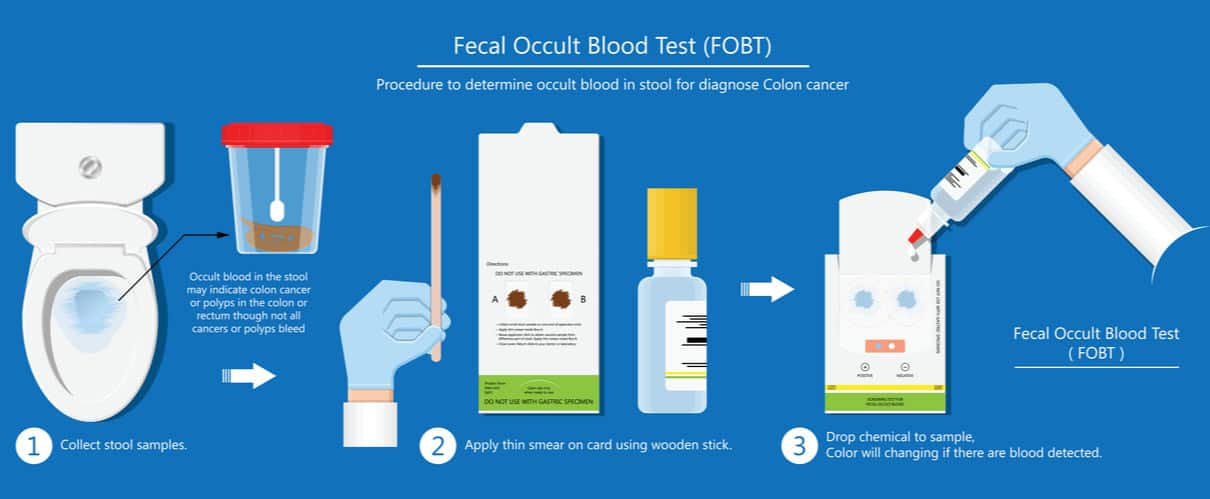
The faecal occult blood test, also called FOBT, is the main screening method recommended in the EU.
There are three types:
- Guaiac FOBT (gFOBT)
This test uses a chemical to detect haem, a component of the blood protein haemoglobin. The chemical will cause a reaction on a paper card to find traces of blood in the stool.
Various foods, dietary supplements and medications can, rarely, affect the results of this faecal occult blood test — either indicating that blood is present when it isn’t (false-positive) or missing the presence of blood that’s actually there (false-negative).
You might be asked to redo the test and to avoid certain foods or medicines before doing it. To ensure accurate test results, follow your doctor’s or the leaflets’ instructions carefully.
- FIT – Faecal Immunochemical Test (or iFOBT)
This test uses specific antibodies to detect human globin protein which is part of haemoglobin. Dietary restrictions are typically not required for FIT and the test can detect the presence of blood at concentrations 100 times lower than can the guaiac test.
- Stool DNA test (also known as a multitargeted stool DNA test or MT-sDNA)
This test currently requires a full faecal stool sample and combines FIT with a test that detects both altered DNA in the stool and small amounts of blood shed into the stool from colon or rectal cancer or polyps. The DNA changes are found in very tiny amounts, so very sensitive laboratory methods are required to detect them. The test is set to be very sensitive and therefore has a higher false positive rate than FIT.
The gFOBT and FIT are widely used and both are proven to indicate the risk of colorectal cancer thus reducing deaths from this disease. However, gFOBT has largely been replaced by the more accurate and sensitive FIT as recommended in the EU guidelines. The FIT is the more accurate of the two and is more likely to detect bleeding polyps than gFOBT.
Both types of test are simple and quick to carry out in the privacy of your home.
How about the results?
- Negative result – A screening test is considered negative if no blood is detected in your stool samples.
- Positive result – A screening test is considered positive if blood is detected in your stool samples and you will need an additional investigation – usually colonoscopy – to look for the source of the (microscopic) bleeding.
When should you start screening?
It is generally recommended that programmes commence screening at age 50 and continue to age 75 sometimes with an option to extend it beyond 75.
Colonoscopy
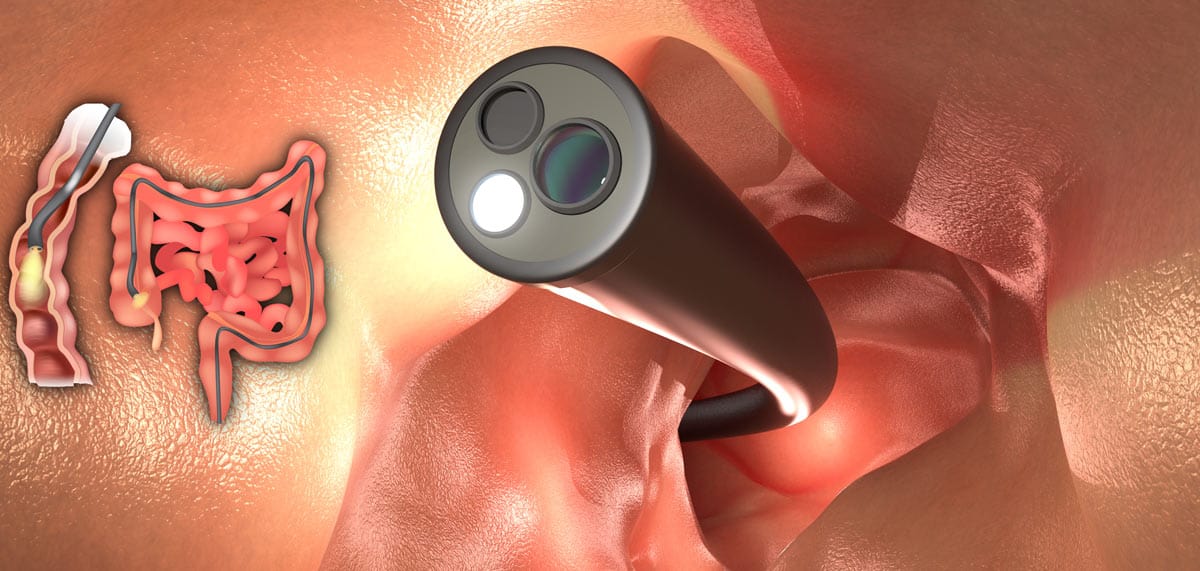
A colonoscopy is another option for colorectal cancer screening. This test is one of the most sensitive currently available as it allows the doctor to directly view the rectum and the entire colon and detect changes or abnormalities in the large intestine (colon) and rectum.
During a colonoscopy a long, flexible tube (colonoscope) is inserted into the rectum.
The scope – which is long enough to reach the entire length of your colon – contains a light and a tube (channel) that allows the doctor to pump air or carbon dioxide into your colon. The air or carbon dioxide inflates the colon which provides a better view of the lining of the colon.
The camera sends images to an external monitor so that the doctor can study the inside of your colon.
Instruments can be inserted through the channel to take tissue samples (biopsies) or remove polyps or other areas of abnormal tissue.
A colonoscopy typically takes about 30 to 60 minutes.
How about the results?
Your doctor will review the results of the colonoscopy and then share the results with you.
- Negative result
A colonoscopy is considered negative if the doctor doesn’t find any abnormalities in the colon
- Positive result
A colonoscopy is considered positive if the doctor finds any polyps or abnormal tissue in the colon
Most polyps are not cancerous, but some can be precancerous. Polyps removed during colonoscopy are sent to a laboratory for analysis to determine whether they are cancerous, precancerous or noncancerous.
How often should this be done?
Most people who have had certain types of polyps removed during a colonoscopy will need to get a colonoscopy again after 3 years, but some people might need to get one earlier (or later) than 3 years, depending on the type, size, and number of polyps.
People who have had colon or rectal cancer may need to have further colonoscopies. Other procedures like ultrasound might also be recommended for some people with rectal cancer, depending on the type of surgery they had.
Flexible Sigmoidoscopy

In this test, the rectum and part of the colon are examined using a flexible lighted instrument which is inserted into the rectum.
This examination is used to evaluate the lower part of the large intestine (colon).
The sigmoidoscope contains a light and a tube (channel) that allows the doctor to pump air or carbon dioxide into your colon. The air expands the colon, which provides a better view of the colon lining.
The instrument also contains a tiny video camera at its tip. The camera sends images to an external monitor so that the doctor can study the inside of your colon. The doctor can also insert instruments through the scope to take tissue samples (biopsies).
A flexible sigmoidoscopy examination typically takes about 15 minutes.
How about the results?
Your doctor will review the results of your flexible sigmoidoscopy examination and then share them with you.
- Negative result.
The results of a flexible sigmoidoscopy exam are considered negative if the doctor doesn’t find any abnormalities in the colon.
- Positive result.
The results of a flexible sigmoidoscopy exam are considered positive if the doctor finds polyps or abnormal tissue in the colon. Depending on the findings you may need additional testing – such as a colonoscopy – so that any abnormalities can be examined more thoroughly, biopsied or removed.
How often should this be done?
If you are at average risk of colorectal cancer – you have no colorectal cancer risk factors other than age – your doctor may recommend waiting five years before repeating the examination.
CT (Computed Tomography) Scan/ Virtual Colonoscopy
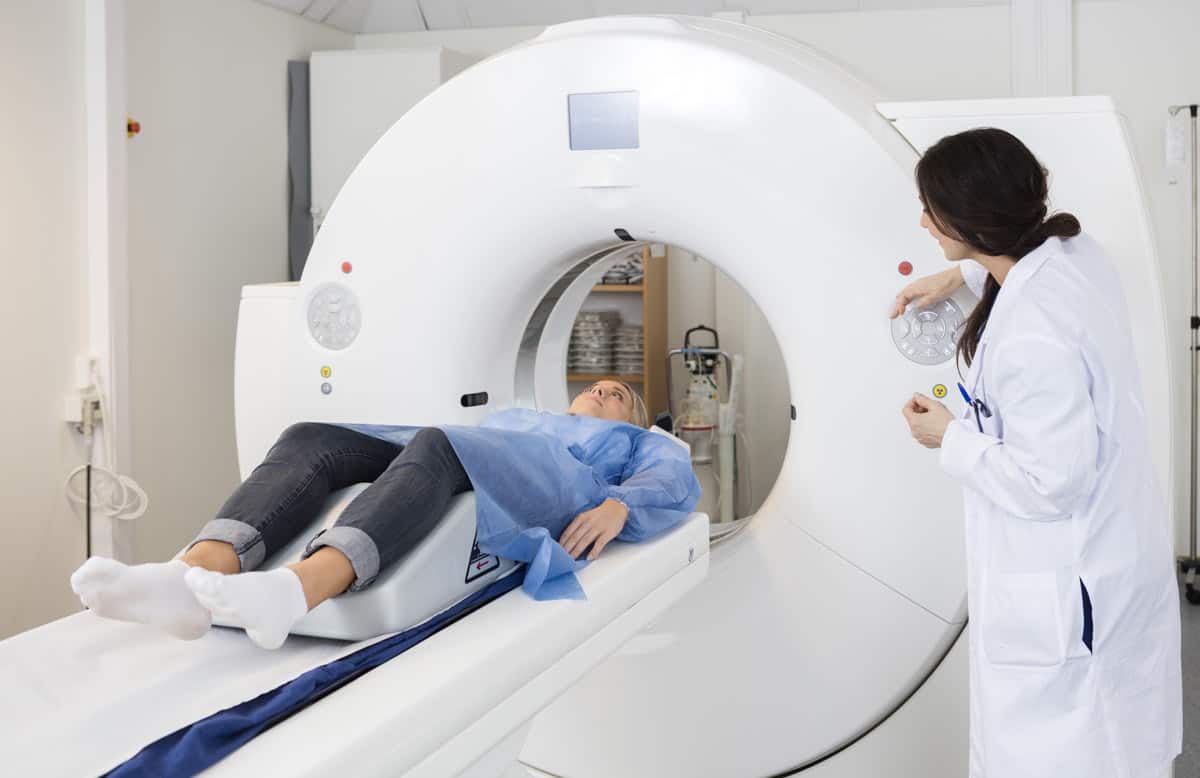
The CT colonography or virtual colonoscopy uses X-Rays and computers to take 2 or 3 dimensional images of the colon and rectum. It is less invasive than a colonoscopy and usually does not require sedation other than a liquid diet and bowel preparation beforehand. Polyps cannot be removed during this screening process which means that a follow up a colonoscopy will be needed if the test is positive.
Depending on the results of the examination re-screening may be needed every 10 years.
Capsule Endoscopy

With capsule endoscopy, a digital video camera with the size and shape of a pill is swallowed to visualise the gastrointestinal tract. It is usually used to examine the small intestine or oesophagus. The procedure requires a liquid diet and bowel preparation. This test is not widely available and is as yet not as effective as colonoscopy in detecting polyps and cancer.
As this is a newer type of test the best length of time to go between tests is not yet clear.

Please confirm if you accept our tracking cookies. When declining the cookies, you can continue visiting the website without sending data to third party services. Read our complete cookie statement here.
